Illustrative Image: Real-World Outcomes of Oral Short-Course Regimen for Rifampicin-Resistant Tuberculosis in High HIV Settings: Insights from South Africa
Image Source & Credit: WHO
Ownership and Usage Policy
A recent study by Stadler et al. (2025) titled “Treatment outcomes with an oral short course regimen for rifampicin-resistant tuberculosis in a high HIV prevalence, programmatic setting in South Africa” published in Clinical Infectious Diseases revealed that although the oral SCR has shown promise in controlled trials, its effectiveness was limited in this high-burden, programmatic setting.
“
Despite rapid culture conversion, oral short-course regimens showed limited success in high HIV, resource-limited settings.– Stadler et al. 2025
The study titled “Treatment Outcomes With an Oral Short Course Regimen for Rifampicin-resistant Tuberculosis in a High HIV Prevalence, Programmatic Setting in South Africa” examines the effectiveness of a fully oral, 7-drug short-course regimen (SCR) that includes bedaquiline and linezolid for treating rifampicin-resistant tuberculosis (RR-TB). Conducted in the Eastern Cape Province—an area with both a high TB burden and significant HIV co-infection rates—the research evaluates real-world treatment performance beyond clinical trials. Key objectives included assessing clinical and bacteriological outcomes, measuring treatment success according to WHO definitions, analyzing TB-free survival at 18 months, monitoring time to sputum culture conversion, and identifying predictors of poor outcomes, particularly in relation to HIV status. Findings revealed that although the oral SCR has shown promise in controlled trials, its effectiveness was limited in this high-burden, programmatic setting. Challenges such as delayed drug resistance testing, restricted access to diagnostic imaging, and overall implementation barriers contributed to underperformance. The study highlights the need for stronger support systems, improved risk stratification, and enhanced patient follow-up to optimize outcomes for RR-TB patients in similar contexts.
How the Study was Conducted
The study was a retrospective cohort analysis conducted in a real-world, programmatic setting in Eastern Cape Province, South Africa—an area with high rates of rifampicin-resistant tuberculosis (RR-TB) and HIV. Data were collected from four decentralized drug-resistant TB treatment sites, with patients enrolled between July 2018 and February 2020. The study population included adults (≥18 years) with newly diagnosed RR-TB who initiated the oral short-course regimen (SCR). Patients with prior second-line TB treatment or confirmed resistance to fluoroquinolones or bedaquiline were excluded. A total of 248 patients met the eligibility criteria.
All participants were treated with a 7-drug, fully oral regimen consisting of bedaquiline, linezolid, levofloxacin, clofazimine, ethambutol, pyrazinamide, and high-dose isoniazid, administered for approximately 9–11 months. Data were obtained from routine programmatic sources, including clinical records, laboratory results (such as sputum cultures and drug susceptibility tests), and HIV-related information (CD4 counts and ART status). Patients were monitored for 18 months after treatment initiation to evaluate TB-free survival. The primary outcome was TB-free survival at 18 months, while secondary outcomes included WHO-defined treatment outcomes (cure, treatment completion, death, or loss to follow-up), time to sputum culture conversion, and identification of predictors of poor outcomes such as age, HIV status, and laboratory markers. The authors employed Kaplan-Meier survival methods and Cox proportional hazards models to assess survival probabilities and determine risk factors associated with unfavorable outcomes.
What the Authors Found
The authors found that while the oral short-course regimen (SCR) for RR-TB achieved rapid bacteriological response (96.8% culture conversion by 90 days), its overall treatment success was low (37.5%), mainly due to high mortality (21.6%) and loss to follow-up (19.4%) in a real-world, high HIV prevalence setting.
Why is this important
Real-World Effectiveness vs. Clinical Trials: The study highlights a significant gap between the strong outcomes seen in controlled clinical trials and the weaker results observed in resource-limited, high-burden settings. Systemic barriers—such as delayed diagnostics and inadequate patient support—limit the real-world impact of promising regimens.
Public Health Significance: With RR-TB being one of the hardest forms of TB to treat, and South Africa facing high HIV co-infection rates, the findings underscore the urgent need to adapt strategies in regions most affected by dual epidemics.
Clinical Insights: Predictors of poor outcomes (older age, low albumin, high bacterial load) can help clinicians identify high-risk patients. Importantly, rapid bacteriological response does not always guarantee long-term treatment success, challenging current metrics of success.
Policy & Program Implications: The study emphasizes that effective treatment requires more than drugs—it depends on stronger health systems. Key priorities include improving diagnostic capacity, providing robust patient support, and strengthening follow-up mechanisms to reduce mortality and loss to follow-up.
What the Authors Recommended
- The study advocates improving patient follow-up mechanisms to reduce loss to follow-up and expanding diagnostic infrastructure (drug susceptibility testing, radiology) to enable timely, accurate treatment decisions.
- The authors ought to use baseline clinical and laboratory markers—such as age, serum albumin, and smear status—to identify high-risk patients and provide tailored monitoring and interventions accordingly.
- Prioritize early ART initiation and adherence support, especially for patients with advanced HIV or low CD4 counts, to improve treatment outcomes.
- Furthermore, regularly evaluate regimen performance in programmatic settings, recognizing that early culture conversion does not always equate to long-term success. Broader indicators should be used to measure effectiveness.
- In addition, modify treatment protocols and support structures to fit the realities of decentralized, resource-limited settings, and ensure new regimens are tested beyond clinical trials before wide-scale implementation.
In conclusion, while the oral short-course regimen demonstrates encouraging bacteriological response, its limited effectiveness in real-world, high HIV prevalence settings underscores the critical importance of strong health systems, timely diagnostics, and tailored patient support. To truly improve outcomes for rifampicin-resistant TB, future strategies must go beyond promising drug regimens and address the structural, clinical, and programmatic barriers that shape patient survival and long-term success.



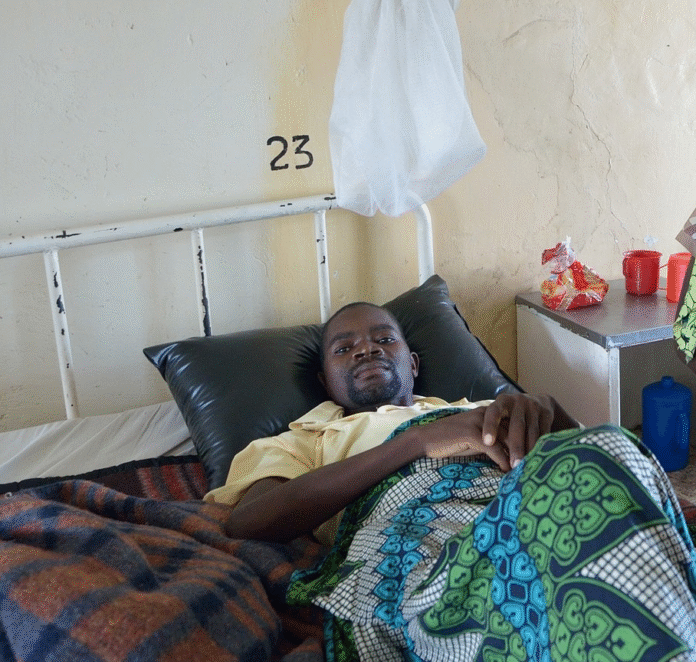












 The African Research (AR) Index is a comprehensive scholarly directory and database focused explicitly on journal publishers that publish and disseminate African research.
The African Research (AR) Index is a comprehensive scholarly directory and database focused explicitly on journal publishers that publish and disseminate African research.

